 7 May, 2026
7 May, 2026
Stentless PCI vs Stent Angioplasty: Understanding the Right Treatment for Heart Blockages | Dr. A B Gopalamurugan
For decades, stent angioplasty has been one of the most widely used treatments for blocked heart arteries. During angioplasty, a narrowed coronary artery is opened to restore blood flow to the heart. In many cases, a small metal mesh tube called a stent is placed inside the artery to keep it open. Modern drug-eluting stents are coated with medicine that helps reduce the chance of re-narrowing.
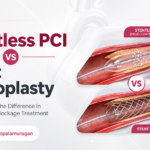
Today, another advanced option is being used in selected patients: Stentless PCI, also known as Drug-Coated Balloon angioplasty or DCB angioplasty. Unlike stent angioplasty, Stentless PCI treats the artery without leaving a permanent metal implant behind. The balloon delivers medicine to the artery wall and is then removed. This is why the approach is often called a “leave nothing behind” angioplasty technique.
But the important question is not simply which treatment is newer. The real question is: which treatment is right for which patient?
Both stent angioplasty and Stentless PCI have an important role in modern cardiology. The right choice depends on the type of blockage, artery size, calcium burden, previous stent history, bleeding risk, heart condition, and the result after lesion preparation.
What Is Stent Angioplasty?
Stent angioplasty is a PCI procedure where a blocked or narrowed coronary artery is opened using a balloon, followed by placement of a stent. The stent acts like a scaffold that supports the artery from inside and helps keep the vessel open.
Modern drug-eluting stents release medicine slowly to reduce tissue growth inside the stent and lower the risk of re-narrowing. Stents are especially useful when the artery needs strong mechanical support, such as in larger arteries, complex blockages, vessel recoil, or dissections after balloon angioplasty.
In many patients, stent angioplasty remains the preferred and most reliable option.
What Is Stentless PCI?
Stentless PCI is a form of angioplasty where the artery is treated without placing a permanent stent.
In this procedure, the cardiologist first prepares the blockage using balloons or specialised devices. Once the artery is opened properly, a Drug-Coated Balloon is inflated inside the vessel. The balloon delivers anti-restenotic medicine to the artery wall and is then removed.
No metal scaffold remains inside the artery.
This approach may help preserve the natural flexibility of the artery and avoid additional metal layers, especially in selected patients with in-stent restenosis, small vessel disease, or situations where leaving less metal behind is desirable. However, Stentless PCI requires careful lesion preparation and is not suitable for every blockage.
Stentless PCI vs Stent Angioplasty: Key Difference
The main difference is simple:
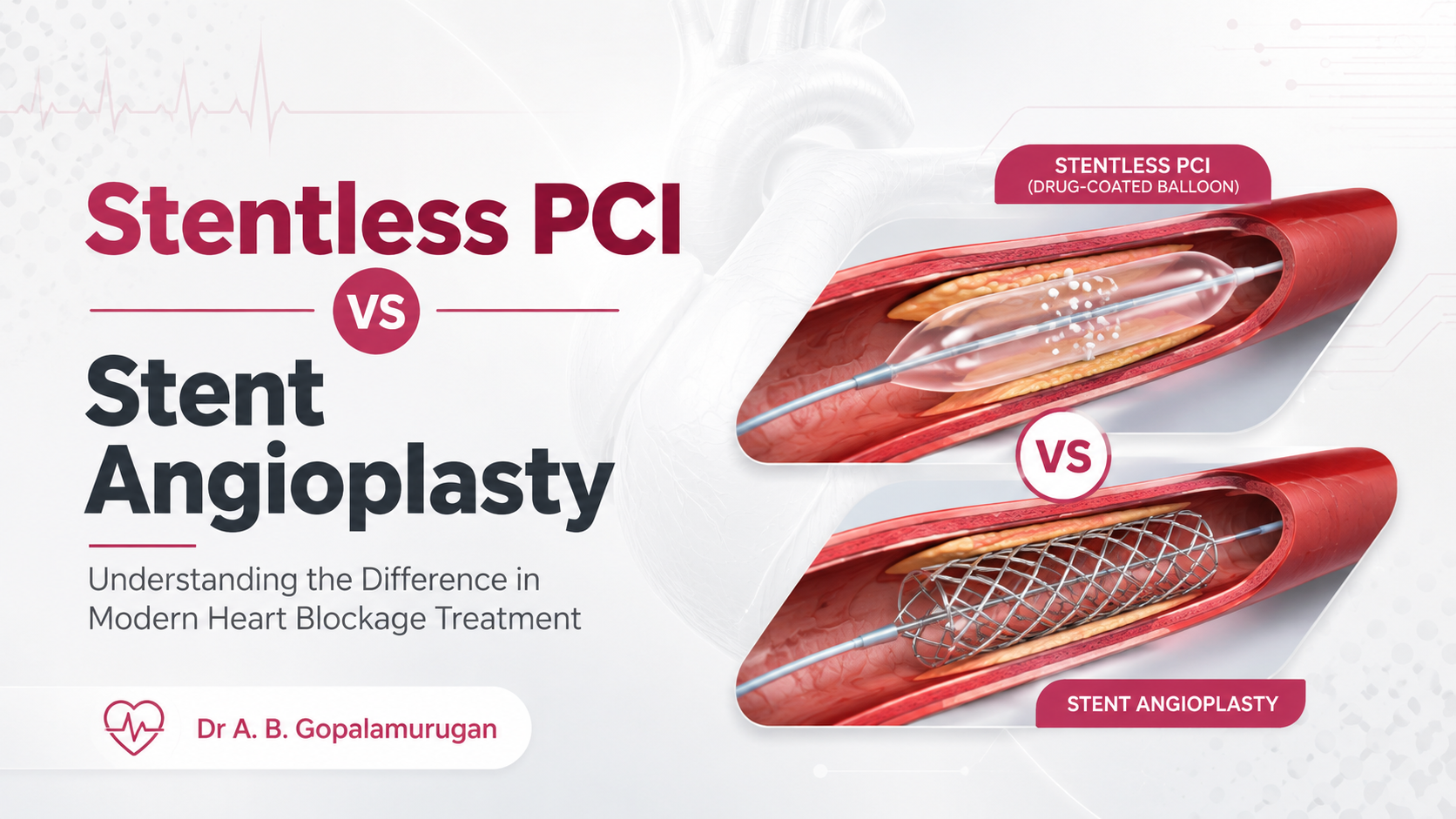
Stent angioplasty leaves a permanent metal scaffold inside the artery. Stentless PCI treats the artery with a drug-coated balloon and leaves no permanent implant behind.
| Feature | Stent Angioplasty | Stentless PCI / DCB Angioplasty |
|---|---|---|
| Permanent implant | Yes, a stent remains inside the artery | No permanent metal implant |
| Main device used | Drug-eluting stent | Drug-coated balloon |
| Mechanical support | Strong support for the artery | No long-term scaffold |
| Common use | Larger vessels, complex lesions, recoil, dissections | In-stent restenosis, small vessels, selected lesions |
| “Leave nothing behind” approach | No | Yes |
| Need for lesion preparation | Important | Extremely important |
| Future treatment flexibility | Can be affected by stent layers | May preserve future options |
| Suitability | Broadly used | Highly case-dependent |
When Is Stent Angioplasty Better?
Stent angioplasty may be better when the artery needs strong support after opening.
This may include:
- Large artery blockages
- Severe vessel recoil after balloon dilatation
- Major dissection after lesion preparation
- Long or complex blockages
- Heavily calcified lesions
- Acute heart attack situations where a stent is clearly required
- Lesions where the artery cannot remain open safely without support
This is why Stentless PCI should not be seen as a complete replacement for all stents. It is a specialised option for carefully selected cases.
When Can Stentless PCI Be Considered?
Stentless PCI may be considered when the cardiologist wants to treat the blockage without adding a permanent metal implant.
It may be suitable for selected patients with:
- In-stent restenosis, where a previous stent has narrowed again
- Small vessel coronary artery disease
- Bifurcation or side-branch lesions
- Patients with multiple previous stents
- High bleeding risk patients
- Patients who may need future surgery
- Selected de novo coronary lesions after good lesion preparation
DCB angioplasty is especially useful in cases where the goal is to treat narrowing without adding another layer of metal inside the artery.
Why Stentless PCI Is Important in India
India has a high burden of coronary artery disease, diabetes, hypertension, and complex heart blockages. Many Indian patients may have small vessel disease, diffuse coronary disease, or repeat narrowing after previous angioplasty.
For such patients, Stentless PCI can be an important treatment option to discuss. It may help selected patients avoid additional metal layers, especially when the blockage is inside a previously placed stent or located in a small artery.
However, the decision must be highly personalised. Not every patient in India with a heart blockage is a candidate for Stentless PCI. The cardiologist must evaluate the angiogram, artery size, lesion type, calcium burden, blood flow, and the final result after vessel preparation.
The Role of Lesion Preparation
The success of Stentless PCI depends heavily on lesion preparation.
Before using a Drug-Coated Balloon, the artery must be opened properly. If the artery does not open well, if there is severe recoil, or if a major dissection occurs, a stent may still be needed.
Lesion preparation may include:
- Balloon pre-dilatation
- Scoring balloon
- Cutting balloon
- High-pressure balloon
- Calcium modification techniques
- OCT or IVUS imaging guidance
DCB-based PCI is not just about using a drug-coated balloon. It is about preparing the artery correctly, assessing the result carefully, and deciding whether it is safe to leave the artery without a stent.
Role of OCT and IVUS in Choosing the Right Treatment
Advanced imaging tools such as OCT and IVUS help cardiologists see the artery from inside. These tools can help assess vessel size, plaque pattern, calcium burden, stent expansion, and the cause of restenosis.
In Stentless PCI, imaging can be useful because the doctor needs to confirm that the artery has opened well and that no major issue requires stent placement.
In stent angioplasty, OCT or IVUS can also help ensure the stent is properly expanded and well positioned.
This means imaging can support both strategies and help doctors choose the safest treatment.
Benefits of Stent Angioplasty
Stent angioplasty has several important advantages:
- Provides strong mechanical support
- Keeps the artery open after balloon angioplasty
- Useful for complex or unstable lesions
- Widely studied and commonly performed
- Preferred in many large-vessel and de novo coronary blockages
- Effective when the artery needs a permanent scaffold
For many patients, stenting remains the most dependable option.
Benefits of Stentless PCI
Stentless PCI may offer benefits in selected cases:
- No permanent metal implant
- Avoids additional stent layers
- Useful for in-stent restenosis
- May be helpful in small vessel disease
- Preserves natural vessel movement
- May keep future treatment options open
- Supports the “leave nothing behind” concept
The biggest advantage is that the artery is treated without leaving a permanent metal cage behind. But this benefit applies only when the artery is suitable and the final angioplasty result is stable.
Limitations of Stentless PCI
Stentless PCI has limitations and should not be used in every patient.
It may not be ideal when there is:
- Severe vessel recoil
- Major dissection
- Heavy calcium that cannot be modified
- Poor blood flow after preparation
- Large artery blockage needing support
- Complex anatomy requiring scaffolding
- Emergency situations where stenting is safer
In these cases, a stent may provide a better and safer result.
Which Is Better: Stentless PCI or Stent Angioplasty?
There is no single answer.
Stent angioplasty is better when the artery needs strong structural support.
Stentless PCI may be better when the artery can be treated safely without leaving metal behind.
The best treatment is not decided by trend or technology alone. It is decided by:
- Patient condition
- Artery size
- Blockage type
- Previous stent history
- Calcium burden
- Bleeding risk
- Imaging findings
- Result after lesion preparation
- Long-term treatment goals
A skilled interventional cardiologist will decide whether the patient needs a stent or whether a stentless approach is possible.
About Dr A. B. Gopalamurugan
Dr A. B. Gopalamurugan is a London-based cardiologist with over 20 years of experience. He is known for his expertise in interventional cardiology, TAVR, electrophysiology, and endovascular aortic repairs.
He has extensive experience in advanced cardiac interventions, including complex coronary procedures, structural heart interventions, and electrophysiology care.
For patients in India considering advanced angioplasty options such as Stentless PCI or DCB angioplasty, expert evaluation is essential to choose the right treatment strategy.
Stentless PCI and stent angioplasty are both valuable treatments for coronary artery blockages. Stent angioplasty remains the standard and preferred option for many patients, especially when the artery needs strong mechanical support. Stentless PCI is a promising and advanced option for selected patients where the artery can be treated without leaving a permanent metal implant.
The key is right patient, right artery, right technique.
For Indian patients with heart blockages, small vessel disease, in-stent restenosis, diabetes-related coronary disease, or previous multiple stents, Stentless PCI may be worth discussing with an experienced interventional cardiologist.
But the final decision should always be based on detailed cardiac evaluation, angiogram findings, imaging when needed, and personalised risk assessment.
FAQs
1. What is the main difference between Stentless PCI and stent angioplasty?
Stent angioplasty places a permanent metal stent inside the artery. Stentless PCI uses a Drug-Coated Balloon to deliver medicine and leaves no permanent metal implant behind.
2. Is Stentless PCI better than stent angioplasty?
Not always. Stentless PCI may be better for selected patients, but stent angioplasty is still better when the artery needs strong support.
3. Who is suitable for Stentless PCI?
Patients with in-stent restenosis, small vessel disease, selected bifurcation lesions, high bleeding risk, or multiple previous stents may be considered for Stentless PCI.
4. Can every heart blockage be treated without a stent?
No. Some blockages require a stent, especially if there is severe recoil, major dissection, heavy calcium, or poor blood flow after balloon treatment.
5. What is DCB angioplasty?
DCB angioplasty means Drug-Coated Balloon angioplasty. It uses a balloon coated with medicine to treat the artery without leaving a stent behind.
6. Is stent angioplasty safe?
Stent angioplasty is a commonly performed and well-established procedure. Like any cardiac procedure, it has risks and benefits that should be discussed with the cardiologist.
7. Is Stentless PCI available in India?
Yes, Stentless PCI and DCB angioplasty are available in selected advanced cardiac centres in India.
8. Does Stentless PCI mean no blood thinners are required?
No. Blood-thinning medicines may still be needed after Stentless PCI. The duration depends on the patient’s condition and the cardiologist’s advice.
9. Why is lesion preparation important in Stentless PCI?
Because there is no stent left behind, the artery must be properly opened before the Drug-Coated Balloon is used. Poor preparation can lead to poor results.
10. How does a cardiologist decide between Stentless PCI and stent angioplasty?
The decision is based on angiogram findings, artery size, blockage type, calcium burden, previous stent history, bleeding risk, imaging findings, and the final result after balloon preparation.
Stentless PCI vs stent angioplasty | stentless PCI India | stent angioplasty India | DCB angioplasty India | Drug-Coated Balloon angioplasty | angioplasty without stent India | coronary angioplasty without stent | stentless heart procedure | leave nothing behind angioplasty | DCB PCI India | drug coated balloon PCI | stent vs balloon angioplasty | stentless PCI benefits | stent angioplasty benefits | who qualifies for stentless PCI | DCB angioplasty candidate | in-stent restenosis treatment India | small vessel coronary artery disease treatment | advanced coronary angioplasty India | OCT guided PCI India | IVUS guided PCI India | complex coronary angioplasty India | heart blockage treatment without stent | best cardiologist for Stentless PCI India | Dr A B Gopalamurugan cardiologist | Dr AB Gopalamurugan Stentless PCI